At Gartside Street Dental Lounge in Manchester city centre, our clinicians share practical guidance to help you make confident treatment decisions.
Gum disease is the most common dental condition in the UK and the leading cause of adult tooth loss, but it is also one of the quietest. Unlike toothache, which announces itself loudly enough to send people to the dentist, gum disease is largely painless until very advanced. The result is that most adults are walking around with some level of gum inflammation without knowing it, and a meaningful proportion are losing bone around their teeth without any obvious symptom. This post explains what gum disease actually is, the stages it moves through, and what to look for so you can catch it before it costs you a tooth.
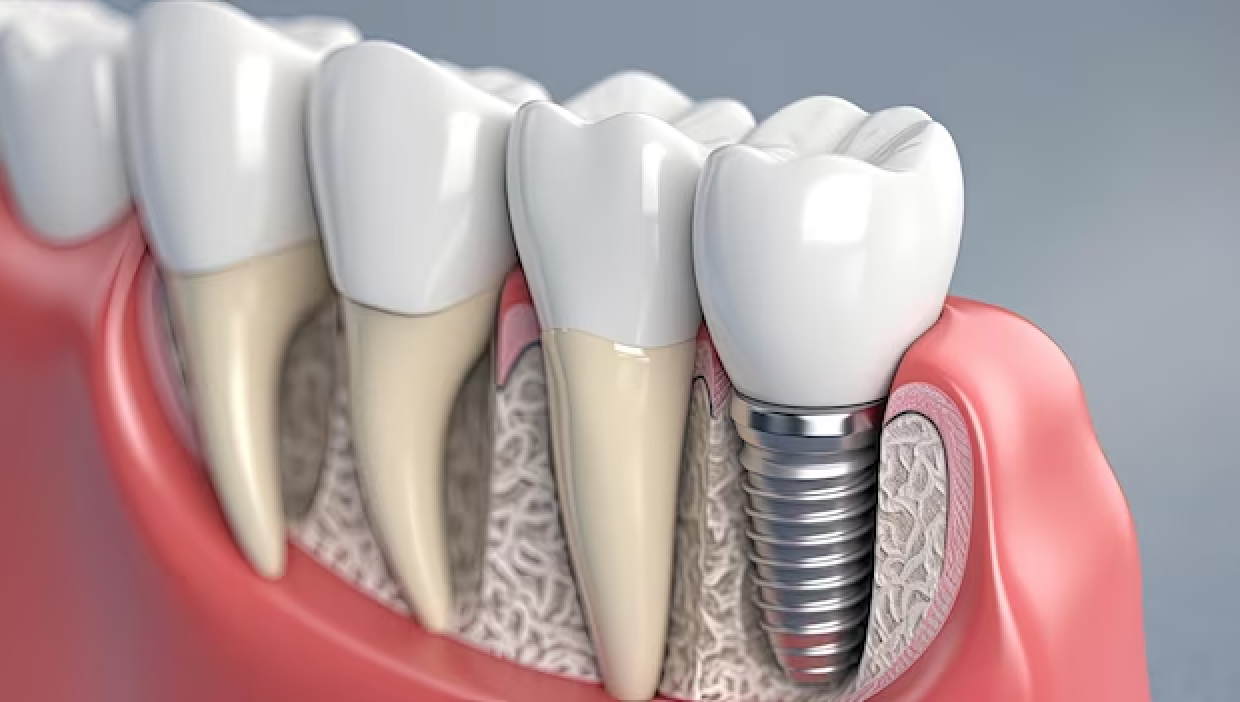
In simple terms, gum disease is a bacterial infection of the gums and the supporting bone, driven by plaque accumulating around the gum line. Inflammation is the body’s response to the bacteria, and over time that inflammation damages first the gum tissue and eventually the bone that holds your teeth in place. The bone, once lost, does not grow back. That is why catching gum disease early matters so much.
The first stage is gingivitis, and it is reversible. The signs are bleeding when you brush or floss, mild redness around the gum margin, and slight puffiness. There is no bone loss yet. Most UK adults experience gingivitis at some point — a survey suggested over half the adult population shows signs of it on examination. The reassuring news is that gingivitis responds quickly to thorough professional cleaning and improved home care. Within a few weeks of consistent daily interdental cleaning and a hygiene visit, healthy gums usually return.
The second stage is early periodontitis. The line between gingivitis and periodontitis is crossed once bone starts to be lost around the teeth. The gum no longer hugs the tooth at the same level — it begins to detach, forming a "pocket" between gum and tooth that traps bacteria. The body cannot fully clear these pockets and the bone slowly erodes. Symptoms remain mild: bleeding still occurs, possibly bad breath, and possibly the start of gum recession. Treatment can stop progression but cannot regrow the bone that has already been lost.
The third stage is moderate to advanced periodontitis. Now bone loss is significant — thirty to fifty per cent or more of the supporting bone may have gone. Pockets deepen, recession becomes visible, teeth may start to drift, food becomes more likely to pack between teeth, and occasional gum abscesses can flare up. Without treatment, teeth eventually become loose and are lost. This stage requires more intensive treatment and lifelong maintenance.
Why is gum disease "silent"? Because the gum bone has no nerves capable of transmitting the kind of warning pain that a toothache provides. The earliest signal the body gives you is bleeding when you brush — the gum’s way of saying it is inflamed. Most people brush around bleeding gums for years rather than treating the bleeding as the warning it is. By the time pain or loose teeth arrive, significant damage has already been done. If your gums bleed regularly when brushing or flossing, that is the moment to act, not the moment to switch to a softer brush.
The signs to watch for, in plain English: bleeding when brushing or flossing, especially regularly. Persistent bad breath. Gums that look red and puffy rather than pink and firm. Visible gum recession, where teeth start to look longer. Gaps appearing between teeth that did not used to be there. Food regularly stuck between teeth in spots that did not used to catch food. Looseness or movement of any tooth. Any one of these is worth a hygiene visit.
Risk factors that meaningfully change the picture. Smoking is the single biggest modifiable risk factor — it multiplies your risk of severe periodontitis by roughly four to five times, and it also masks bleeding, so smokers often have advanced disease before any symptom appears. Poorly controlled diabetes increases risk significantly. Genetics plays a role, which is why some people with excellent oral hygiene still develop periodontitis and others with mediocre habits do not. Stress, certain medications (especially those that reduce saliva flow), pregnancy hormones, and ageing also increase susceptibility.
There is reasonable evidence linking periodontal disease to broader systemic health, although we try not to oversell it. The strongest links are with cardiovascular disease (the proposed mechanism is chronic low-grade inflammation), with diabetes (the relationship is bidirectional — gum disease worsens blood sugar control and vice versa), and with adverse pregnancy outcomes including preterm birth. There are weaker associations with other conditions including some neurodegenerative diseases. Reducing chronic mouth inflammation is a sensible health investment regardless of which downstream link you find most compelling.
Treatment moves up a ladder depending on severity. For gingivitis: a thorough scale and polish to remove plaque and tartar, plus dedicated time to teach you the right brushing and interdental cleaning technique for your mouth. Often the inflammation resolves within a few weeks of better home care. Hygiene visits at three- to six-monthly intervals catch any return early. For early periodontitis: root surface debridement (sometimes called RSD or "deep cleaning"). This involves cleaning the root surfaces below the gum line under local anaesthetic, usually quadrant by quadrant over two to four visits. The goal is to remove the bacterial reservoir trapped in the pockets so the gum can reattach and inflammation can settle. RSD is a non-surgical procedure carried out by hygienists or dentists with specific training, and is the workhorse treatment for early-to-moderate periodontitis.
For moderate to advanced periodontitis, treatment may extend to surgical procedures (such as flap surgery to access deeper pockets), regenerative techniques in selected sites, or referral to a periodontal specialist. We will refer when we believe specialist input will give a better outcome. Regardless of the surgical detail, the foundation is always the same: bacterial control through home care, supported by frequent professional maintenance.
Home care is where most gum disease is won or lost, and the single most important point is that brushing alone is not enough. The majority of gum disease starts between teeth, where a toothbrush physically cannot reach. Interdental brushes — the small thin brushes in graded sizes — are usually more effective for adults than floss, because they are easier to use correctly and clean more thoroughly. Electric toothbrushes outperform manual brushes for most users, particularly oscillating-rotating and sonic types. Technique matters more than enthusiasm; we will demonstrate exactly what works for your mouth at a hygiene visit.
The bigger point about gum disease is that once you have had it, you remain at higher risk for life. Stopping the disease in its tracks at age forty does not mean you can return to brushing twice a day and check-ups every six months. It means three- or four-monthly hygiene visits, careful daily home care, and ongoing monitoring of pocket depths. This is not a one-time fix — it is a long-term maintenance relationship.
If your gums bleed when you brush, even occasionally, do not ignore it. A hygiene visit is one of the cheapest, lowest-anxiety, highest-leverage things you can do for your long-term dental health. Book an assessment and we will tell you honestly where you are on the spectrum and what (if anything) needs doing. Ready to Transform Your Smile?
Take the first step towards your dream smile. Book a free consultation with our expert team at our Manchester clinic and discover how we can help you achieve the confidence you deserve.